Accurate medical coding is the backbone of healthcare billing, and when it comes to complex conditions like AIDS, precision becomes even more important. Understanding the icd-10 code for aids is essential for healthcare providers, coders, and billing professionals who want to ensure proper reimbursement and compliance with regulations. This article breaks down the topic in a clear, practical way so you can apply it confidently in real-world billing scenarios.
Understanding AIDS in Medical Coding

Acquired Immunodeficiency Syndrome (AIDS) is the advanced stage of HIV infection. It severely weakens the immune system, making the body vulnerable to opportunistic infections and certain cancers. From a billing perspective, AIDS is not just a clinical diagnosis—it carries specific coding requirements that affect claims processing, reimbursement, and reporting.
Medical coding systems like ICD-10 are designed to standardize how diseases are recorded across healthcare systems. This ensures consistency in patient records, insurance claims, and public health data.
What Is the ICD-10 Code for AIDS
The primary icd-10 code for aids is:
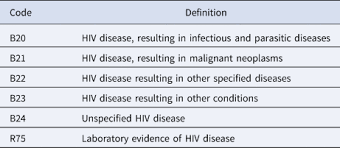
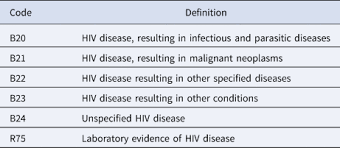
B20 – Human immunodeficiency virus [HIV] disease
This code is used when a patient has confirmed HIV infection and has developed symptoms or complications associated with AIDS. It reflects a more advanced stage of HIV where the immune system is significantly compromised.
It’s important to note that once a patient is diagnosed with AIDS (B20), they will always be coded under B20 in future encounters, even if symptoms are not currently present.
Difference Between HIV and AIDS Coding
A common source of confusion in billing is the distinction between HIV-positive status and AIDS.
Z21 – Asymptomatic HIV infection status
Used when a patient is HIV-positive but has no symptoms or AIDS-related conditions.
B20 – HIV disease (AIDS)
Used when the patient has developed symptoms, opportunistic infections, or conditions linked to HIV.
This distinction is critical because incorrect coding can lead to claim denials or compliance issues. For example, coding Z21 instead of B20 for a symptomatic patient would be inaccurate and may result in underpayment.
When to Use the ICD-10 Code for AIDS
The icd-10 code for aids (B20) should be used in the following situations:
When the patient has documented HIV disease with symptoms
When there are AIDS-defining conditions such as opportunistic infections
When the provider explicitly documents AIDS or HIV disease
When the patient has a history of HIV-related illness
Coders should rely on provider documentation and not assume a diagnosis. If documentation is unclear, it is always best to query the provider.
Common AIDS-Related Conditions to Code Alongside B20
Patients with AIDS often present with additional conditions. These must be coded separately to provide a complete clinical picture and ensure proper reimbursement.
Examples include:
Tuberculosis
Pneumocystis pneumonia
Kaposi’s sarcoma
Candidiasis
Cytomegalovirus infection
When coding, B20 is listed first, followed by codes for the specific conditions. This sequencing reflects that AIDS is the underlying cause of these complications.
Importance of Accurate Coding in Healthcare Billing
Using the correct icd-10 code for aids directly impacts revenue cycle management. Here’s why it matters:
Proper reimbursement
Insurance companies rely on accurate codes to determine payment. Incorrect coding can lead to denied or reduced claims.
Compliance and audits
Regulatory bodies closely monitor coding practices. Errors in HIV/AIDS coding can trigger audits or penalties.
Clinical data accuracy
Accurate coding contributes to reliable healthcare statistics and patient care planning.
Risk adjustment
Patients with AIDS often fall into higher risk categories, which can affect reimbursement models in value-based care.
Documentation Tips for Coders
Good documentation is essential for correct coding. Coders should look for:
Clear mention of HIV disease or AIDS
Details of related conditions or infections
Physician confirmation of diagnosis
History of HIV-related illness
Avoid coding based on lab results alone unless the provider has confirmed the diagnosis. Coding must always reflect documented clinical judgment.
Common Coding Mistakes to Avoid
Even experienced coders can make errors when dealing with HIV and AIDS codes. Some common mistakes include:
Using Z21 for symptomatic patients
Failing to code related conditions
Incorrect sequencing of codes
Coding suspected cases without confirmation
Not updating codes when the patient progresses from HIV to AIDS
Avoiding these mistakes improves claim accuracy and reduces delays in payment.
Billing Challenges with AIDS Cases
Healthcare billing for AIDS patients can be complex due to multiple factors:
Frequent hospital visits
Multiple comorbidities
Long-term treatment plans
Specialized medications
Each of these elements must be reflected in the coding to ensure proper reimbursement. Missing even one component can result in incomplete claims.
Role of Coders in Managing AIDS Claims
Medical coders play a crucial role in ensuring that AIDS-related claims are processed correctly. Their responsibilities include:
Reviewing medical records thoroughly
Applying the correct ICD-10 codes
Ensuring proper sequencing
Communicating with providers for clarification
Staying updated with coding guidelines
A skilled coder can significantly reduce claim denials and improve billing efficiency.
Updates and Guidelines to Watch
ICD-10 codes are periodically updated, and coding guidelines evolve. Coders should stay informed about:
Official coding guidelines for HIV and AIDS
Changes in documentation requirements
Updates in payer policies
New treatment protocols that may affect coding
Regular training and reference to official resources help maintain accuracy.
Real-World Example of Coding
Consider a patient diagnosed with AIDS who is admitted for Pneumocystis pneumonia.
Correct coding would be:
B20 – HIV disease
Followed by the code for Pneumocystis pneumonia
This sequencing ensures that the primary condition (AIDS) is recognized as the underlying cause.
Why the ICD-10 Code for AIDS Matters Beyond Billing
While billing is the primary focus, the icd-10 code for aids also plays a role in:
Public health tracking
Research and epidemiology
Resource allocation in healthcare systems
Policy-making decisions
Accurate coding contributes to a broader understanding of disease patterns and healthcare needs.
Frequently Asked Questions
What is the ICD-10 code for AIDS
The ICD-10 code for AIDS is B20, which represents HIV disease with symptoms or complications.
Can Z21 and B20 be used together
No, Z21 and B20 should not be used together. Once a patient is diagnosed with AIDS, only B20 is used.
Is B20 used for all HIV patients
No, B20 is only used for patients with symptomatic HIV or AIDS. Asymptomatic patients are coded with Z21.
Do I need to code opportunistic infections separately
Yes, all related conditions should be coded separately after B20 to provide a complete clinical picture.
Can AIDS be coded without provider confirmation
No, coders must rely on provider documentation. Suspected or possible cases should not be coded as confirmed AIDS.
Does the ICD-10 code for AIDS change over time
The code B20 remains standard, but guidelines and documentation requirements may change, so staying updated is important.
Why is sequencing important in AIDS coding
Proper sequencing ensures that the underlying condition (AIDS) is recognized first, which affects reimbursement and claim processing.
What happens if the wrong code is used
Incorrect coding can lead to claim denials, delayed payments, or compliance issues.
Final Thoughts
Understanding the icd-10 code for aids is more than just memorizing a code—it’s about applying it correctly in real-world scenarios. Accurate coding ensures that healthcare providers are reimbursed properly, patients’ records are complete, and the healthcare system functions efficiently. By focusing on proper documentation, correct sequencing, and staying updated with guidelines, billing professionals can handle AIDS-related claims with confidence and accuracy.
read more