Fatty liver disease has become increasingly common across the globe, driven by lifestyle changes, rising obesity rates, and metabolic disorders. For healthcare providers, medical coders, and billing professionals, accurate diagnosis coding is essential—not just for compliance, but also for proper reimbursement and patient care documentation. Understanding the ICD-10 code for fatty liver is a crucial part of this process.
This guide explains fatty liver disease, its classification, and how to use the correct ICD-10 codes in real-world medical coding scenarios. Whether you are a beginner or an experienced coder, clarity in coding can prevent claim denials and improve healthcare data accuracy.
Understanding Fatty Liver Disease

Fatty liver disease occurs when excess fat accumulates in liver cells. It is generally categorized into two main types:
Non-alcoholic fatty liver disease (NAFLD)
This type is not caused by alcohol consumption. It is commonly linked with obesity, diabetes, high cholesterol, and metabolic syndrome.
Alcoholic fatty liver disease (AFLD)
This type results from excessive alcohol intake and can progress to more severe liver conditions if untreated.
Fatty liver often shows no symptoms in early stages, which makes proper documentation and coding even more important when it is diagnosed.
Importance of Accurate ICD-10 Coding
ICD-10 coding is not just about assigning numbers—it reflects the patient’s condition, supports clinical decisions, and ensures proper billing. Using the correct ICD 10 code for fatty liver helps in:
Accurate reimbursement from insurance providers
Maintaining proper medical records
Supporting epidemiological research and reporting
Avoiding claim rejections and audits
Incorrect coding can lead to financial losses and compliance issues, so precision matters.
ICD-10 Code for Fatty Liver
The primary ICD-10 code used for fatty liver is:
K76.0 – Fatty (change of) liver, not elsewhere classified
This is the most commonly used code when documenting non-specific fatty liver conditions, especially in cases where alcohol is not the primary cause or when the documentation does not clearly specify the type.
However, fatty liver can fall under different codes depending on its cause and severity.
Related ICD-10 Codes for Fatty Liver Conditions
Medical coders should always review clinical documentation carefully before assigning a code. Here are some related codes that may apply:
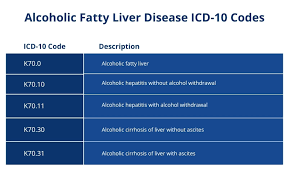
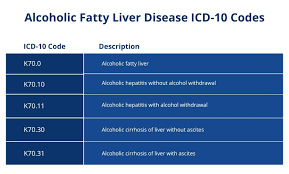
K70.0 – Alcoholic fatty liver
Used when fatty liver is directly linked to alcohol consumption.
K76.0 – Non-alcoholic fatty liver (unspecified)
Used for general fatty liver diagnosis when no specific classification is mentioned.
K75.81 – Nonalcoholic steatohepatitis (NASH)
This is a more advanced form of NAFLD involving inflammation and liver damage.
K74.60 – Unspecified cirrhosis of liver
Used if fatty liver progresses to cirrhosis without clear specification.
E66.9 – Obesity, unspecified
Often coded alongside fatty liver as a contributing condition.
E11.9 – Type 2 diabetes mellitus without complications
Another common comorbidity associated with fatty liver disease.
Assigning multiple codes may be necessary to reflect the complete clinical picture.
When to Use K76.0 Code
The ICD 10 code for fatty liver (K76.0) should be used when:
The diagnosis clearly states fatty liver without specifying alcohol involvement
There is no mention of inflammation (which would suggest NASH)
The condition is identified through imaging or lab results without complications
Coders must avoid assumptions. If documentation is unclear, it is best practice to query the healthcare provider.
Documentation Tips for Accurate Coding
Proper documentation is the backbone of accurate coding. Healthcare providers should include:
Type of fatty liver (alcoholic or non-alcoholic)
Severity and stage of the disease
Associated conditions like obesity or diabetes
Diagnostic methods such as ultrasound or biopsy
Clear and detailed documentation reduces ambiguity and ensures the correct ICD-10 code is assigned.
Common Coding Mistakes to Avoid
Even experienced coders can make errors when handling fatty liver cases. Some common mistakes include:
Using K76.0 when the condition is alcoholic in nature
Failing to code associated conditions like diabetes or obesity
Misclassifying NASH as simple fatty liver
Ignoring physician notes that clarify the cause
Avoiding these mistakes improves coding accuracy and reduces claim denials.
Clinical Significance of Fatty Liver Coding
Accurate coding is not just administrative—it plays a role in patient care. Fatty liver disease can progress to serious conditions such as liver fibrosis, cirrhosis, or even liver cancer if not managed properly.
By using the correct ICD 10 code for fatty liver, healthcare systems can:
Track disease prevalence
Identify high-risk populations
Improve treatment planning
Support research and healthcare policy decisions
Fatty Liver and Comorbidities
Fatty liver rarely exists in isolation. It is often linked with:
Obesity
Type 2 diabetes
Hypertension
High cholesterol
Coders should capture all relevant conditions to provide a complete clinical picture. This not only supports better patient care but also ensures appropriate reimbursement.
Tips for Medical Coders
To improve accuracy when coding fatty liver cases:
Always review the full patient record
Look for keywords like “alcoholic,” “non-alcoholic,” or “NASH”
Verify lab reports and imaging results
Query physicians when documentation is unclear
Stay updated with ICD-10 coding guidelines
Consistency and attention to detail are key to becoming a skilled medical coder.
Future Trends in Fatty Liver Coding
With the rise in lifestyle-related diseases, fatty liver cases are expected to increase. This means coding professionals will play an even more important role in healthcare documentation.
Advancements in electronic health records (EHR) and AI-assisted coding tools may improve accuracy, but human expertise will remain essential for interpreting complex medical data.
Conclusion
Fatty liver disease is a growing health concern, and accurate medical coding is critical for effective healthcare management. Understanding the correct ICD 10 code for fatty liver, especially K76.0 and its related codes, ensures proper documentation, billing, and patient care.
Medical coders must rely on detailed clinical documentation, stay updated with coding standards, and avoid common mistakes to maintain accuracy. As healthcare continues to evolve, precise coding will remain a vital component of the system.
Frequently Asked Questions (FAQ)
What is the ICD 10 code for fatty liver
The most commonly used code is K76.0, which refers to fatty liver not elsewhere classified.
What is the difference between K70.0 and K76.0
K70.0 is used for alcoholic fatty liver, while K76.0 is used for non-alcoholic or unspecified fatty liver.
Can fatty liver be coded with other conditions
Yes, it is often coded with related conditions like obesity, diabetes, or metabolic syndrome.
What is NASH and how is it coded
Nonalcoholic steatohepatitis (NASH) is a more severe form of fatty liver and is coded as K75.81.
Why is accurate coding important for fatty liver
Accurate coding ensures proper billing, supports clinical care, and helps in tracking disease trends.
When should a coder query a physician
A coder should query when the documentation does not clearly specify the type or cause of fatty liver.
Is fatty liver a serious condition
It can be, especially if it progresses to inflammation, fibrosis, or cirrhosis.
Do all fatty liver cases use K76.0
No, the code depends on the cause and severity. Alcoholic and advanced cases use different codes.
read more